
Epidemiology and classification of autoimmune thyroid diseases
Identified in 1956, autoimmune thyroid diseases are considered organ-specific diseases.
They are very frequent; their prevalence changes considerably according to gender, age, race and also geographic area. They prevail among women and generally develop in middle-aged patients. They show a family predisposition.
This is how they can be classified:
- Diffuse lymphocytic thyroidites
- classic Hashimoto's thyroiditis
- idiopathic myxedema
- asymptomatic atrophic thyroiditis - Primary hyperthyroidism
- with/without goiter
- with/without eye disease
- with/without pretibial myxedema
They also include what are known as focal lymphocytic thyroidites, which are not autoimmune thyroid diseases, but which can have single or multifocal lymphocytic infiltrates and, as a consequence, can result to be positive at the autoantibody tests.
Finally, the classification can also include two additional clinical conditions, that are closely correlated with the autoimmune thyroid diseases and are considered to be diseases of probable autoimmune etiology: i.e. endocrine eye disease and pretibial myxedema.
Thyroid antigen-antibody systems
The main autoantibodies are directed against:
- thyroglobulin
- cytoplasmic antigens
- thyroid hormones and TSH
- TSH receptor
- retrobulbar tissue antigens
ANTIBODIES AGAINST THYROGLOBULIN AND CYTOPLASMIC ANTIGENS
Anti-thyroglobulin (anti-TG) autoantibodies
Mainly of class IgG, they are organ- and not strictly species-specific.
In 1956 it was found that TG could be considered an autoantigen. TG is the main iodated protein synthetized by thyrocytes and then stored as a hormone reservoir in the thyroid follicle, codified by a gene present in chromosome 8.
It is a water-soluble glycoprotein made up of 2 dimers, the amino acid sequence of which has been fully identified; despite its large dimensions, only 10 autoantigenic epitopes have been identified.
Both patients with lymphocytic thyroiditis and healthy subjects with anti-TG autoantibodies recognize strictly species-specific epitopes present in the most conserved portion of the molecule, coinciding with the T3 and T4 hormonogenetic part.
Anti-TG antibodies have been identified (see fig.1):
1. in patients with autoimmune thyroid diseases
2. in patients with non-autoimmune thyroid diseases
3. in patients without clinical thyroid diseases.
They are almost always present in association with thyroid anti-microsomal antibodies and it is rare to find a subject only having anti-TG antibodies.
Anti-thyroperoxidase (anti-TPO) autoantibodies
Mainly of class IgG, they are organ- and not strictly species-specific.
In 1957, they were found to react against a scarcely glycosylated cytoplasmic antigen, which is particularly abundant on the apical margin of the thyrocyte, intimately bound to the smooth endoplasmic reticulum, making up the cell membrane, and identified with the microsomal fraction. In 1985 they were identified with thyroid peroxidase (TPO), a transmembrane protein codified by a gene located on chromosome 2, responsible for iodation and the insertion of thyrosine residues in the TG, with at least 6 autoantigenic epitopes.
Anti-TPO autoantibodies react both against conformational epitopes and linear determinants; one of these epitopes is shared with TG and, for this reason, it is called anti-TGPO.
Anti-TPO antibodies have been found (see fig.1):
4. in patients with autoimmune thyroid diseases
5. in patients with non-autoimmune thyroid diseases
6. in patients without clinical thyroid diseases.
Their assay is of fundamental importance, as they can be identified in most patients with Hashimoto’s thyroiditis, their titer correlates with the active phases of the disease and, moreover, they cause direct damage to thyrocytes through complement and K-cell activation.
Anti-TPO and anti-TG antibodies in patients with autoimmune thyroid diseases, non autoimmune thryoid diseases and in controls
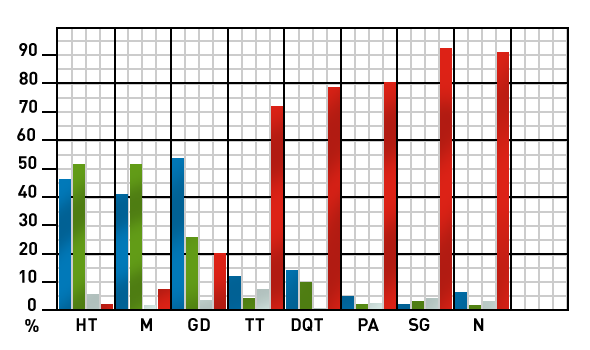
| HT = Hashimoto’s thyroiditis M = Myxedema GD = Graves Disease TT = Thyroid Tumors DQT = De Quervain’s Thyroiditis PA = Plummer’s Adenoma SG = Simple Goiter N = Normal |
As already mentioned, a study carried out on a population of hospitalized subjects without clinical thyroid diseases has demonstrated that there is a correlation between anti-thyroid antibodies and the presence of thyroid lymphocytic infiltrates (see fig.2).
Anti-thyroid antibodies in subjects without clinical thyroid diseases
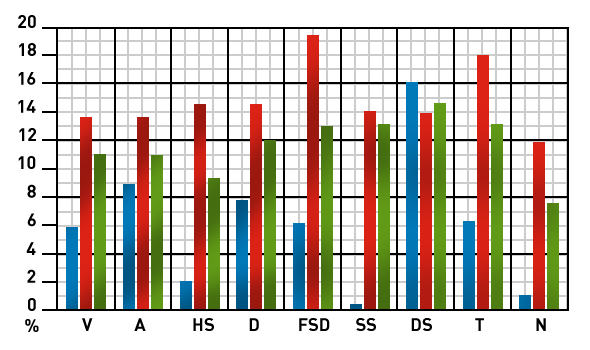
| V = Vitiligo A = Alopecia HS = Hospitalized Subjects D = Ins.Dep. Diabetes Mellitus FSD = First Stage IDDM SS = Sjögren’s Syndrome DS = Down’s Syndrome T = Total N = Normal |
Conclusions: when to request them?
Today, the search for anti-thyroid antibodies has become an unrenounceable lab investigation for clinicians and to reach a final diagnosis of autoimmune or non-autoimmune thyroid disease.
Furthermore, the possibility to quantify the Tg and TPO concentration allows the monitoring of the active phase of the disease and its course.
Hence, the conditions in which requesting anti-TPO and anti-TG assessment is advisable are listed below:
- hypothyroidism (clinical, subclinical)
- hyperthyroidism (clinical, subclinical)
- goiter (especially if of recent onset and increased size)
- thyroid nodules
- isolated endocrine eye disease
- familiarity for autoimmune thyroid diseases
- organ-specific autoimmune diseases
- intermediate autoimmune diseases
- chromosomal abnormalities (Turner’s syndrome, Down’s syndrome)
- before or during treatment with interferon
- 7644 Eu-Tg
EIA for the detection of IgG autoantibodies anti thyroglobulin (Tg) - 7645 Eu-TPO
EIA for the detection of IgG autoantibodies anti thyroid peroxidase (TPO) - 7666 Eu-Thyroglobulin
EIA for the detection of thyroglobulin (hTG)

